This video can not be played
To play this video you need to enable JavaScript in your browser.
Health officials are urging parents to look out for symptoms of Strep A after six children died with an invasive form of the bacterial infection.
Strep A infections are usually mild, causing illness ranging from a sore throat to scarlet fever, but can develop into a more serious invasive Group A Strep (iGAS) infection.
Experts say there are more Strep A cases than usual this year.
Prof Beate Kampmann said parents should seek medical help if they were worried.
Health officials confirmed on Friday that six children had died with iGAS – including five under 10-year-olds in England and a girl from Wales – since September. No deaths have been confirmed in Scotland or Northern Ireland.
The UK Health Security Agency said the last time there was an intensive period of Strep A infection was in 2017-18, when there were four deaths in England in the equivalent time frame.
The rise in Strep A cases and deaths is most likely due to high amounts of the bacteria circulating and increased social mixing, the UKHSA said.
Speaking to BBC Radio 4’s Today programme on Saturday, infectious diseases paediatrician Prof Kampmann said Strep A caused “an asymptomatic infection in the majority of people, then there is a sore throat, then scarlet fever, and in a very, very small minority will there be invasive Group A Strep”.
She said there had been three times as much scarlet fever this year than was seen pre-pandemic: “It starts off with a high fever, very sore throat and very red tongue, which has this sort of papillae – eventually developing a rash which feels a bit like sandpaper.
“The rash starts in the elbows and behind the neck. It tends to then peel after about 10 days because the disease is caused by a toxin that is produced by this bacterium.”
Prof Kampmann said if children became really unwell, or if parents were in doubt, they should seek help. She also said children with a fever should be kept off school.
She continued: “The good news is that Group A Strep is very, very treatable with penicillin.”
But she added, “if your child is deteriorating in any way, you feel that they’re not eating, drinking, being quite flat and lethargic you need to take them to the doctors and to get them checked out”.
The latest data shows there were 851 cases of scarlet fever reported in the week of 14-20 November, compared to an average of 186 for the preceding years.
Virologist Dr Chris Smith said the general rise in Strep A infections could be due to a drop in immunity following the pandemic.
He told BBC Breakfast: “There’s something about the vulnerability of the population and particularly younger people.
“What has changed is that younger people have been through three years, almost, of relative isolation from each other.
“They haven’t caught the normal infections at the normal rates and at the normal times that normal children of that sort of age bracket would have done.
“So, we wonder whether it is that we are seeing a big rash of cases all at once.”
There have been 2.3 cases of the invasive Strep A disease per 100,000 children aged one to four in England this year, compared with an average of 0.5 in pre-pandemic seasons of 2017-19, the UKHSA said.
There have also been 1.1 cases per 100,000 children aged five to nine, compared with a pre-pandemic average over the same period of 0.3.
UKHSA advises people to call 999 or go to A&E if:
- your child is having difficulty breathing – you may notice grunting noises or their tummy sucking under their ribs
- there are pauses when your child breathes
- your child’s skin, tongue or lips are blue
- your child is floppy and will not wake up or stay awake

What is Strep A?
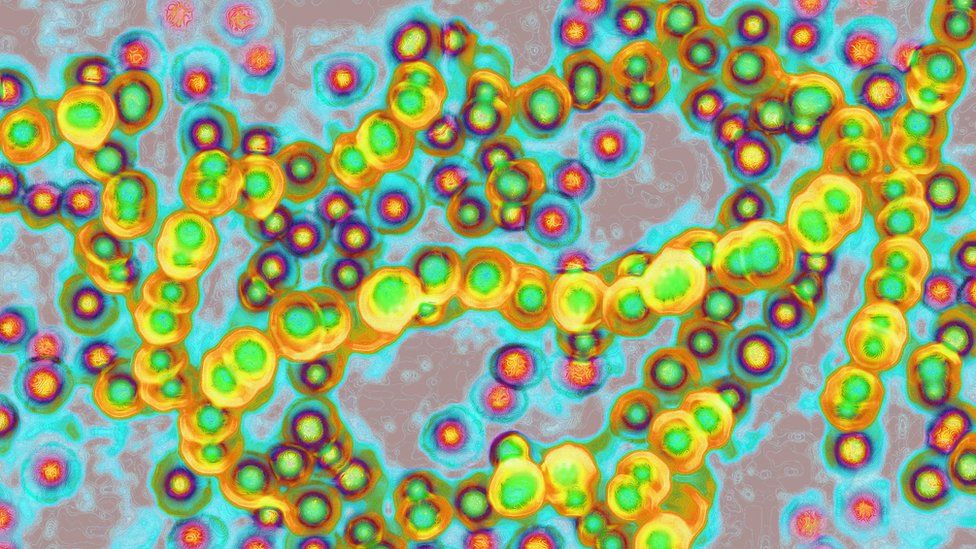
- Group A streptococcal (GAS) infection is caused by strains of the streptococcus pyogenes bacterium
- The bacteria can live on hands or the throat for long enough to allow easy spread between people through sneezing, kissing and skin contact
- Most infections cause mild illnesses such as “strep throat” or skin infections
- It can also cause scarlet fever and in the majority of cases this clears up with antibiotics
- On rare occasions the bacteria can get deeper into the body – including infecting the lungs and bloodstream. It is known as invasive GAS (iGAS) and needs urgent treatment as this can be serious and life-threatening

-
-
19 hours ago

-
-
-
23 hours ago

-
